Life Restarted at 33 – A Sudden Cardiac Arrest Survival Story
I’m so honored to be able to share this story of a life restarted at 33 years of age, as told by my friend Angela who is sharing with us today her personal Sudden Cardiac Arrest survival story.
The following is a true story that has so moved me, that I asked Angela to share it with all of you. Before she shared her story with me, Angela just seemed like another happy, beautiful sports mama friends of mine. I only learned of Angela’s heart incident and history after our kids had a fellow teammate collapse from a heart issue and by the grace of God – and the quick action of a gym worker – his life was saved thanks to the fact that this person knew CPR. As you will learn with Angela’s story, CPR played a major roll in her survival as well.
I think that we can all learn so much for Angela’s personal experience and I am beyond grateful for the fact that she is so willing to educate and share.
Here is Angela’s story, in her own words:
A lot of people use the acronym ‘YOLO’ (You Only Live Once) and really have done some amazing things with that mindset. There’s also a group of people who can say ‘YOLT’ for You Only Live Twice and if they are lucky enough to, can I’m one of those people and here is my story.
I was diagnosed with a bicuspid aortic valve at 19, doctors believe was due to a congenital defect, where two of the three leaflets of my aortic valve fused together sometime before I was born. Most people with BAV do not experience symptoms until adulthood, similar to fatigue, dizziness, or a murmur picked up by a doctors visit, as how mine was found.
Now, being the know-it-all 19 year old I was when I was given this diagnosis by myself from a cardiologist lacking some bedside manner, who told me I could never have children, and that due to my height and thinness (I was MUCH skinnier back in those days) I might have Marfans Syndrome, a connective tissue disorder that can affect the eyes, skeleton, blood vessels, and you guessed it, the heart. He said I may need genetic testing to confirm if I even have it and if that’s what caused my BAV. I was shocked and scared and I left not sure about following any his guidance to come back later for medical help at a yearly follow up, but I did reach out to a genetic counselor about the Marfan’s. I had what seemed like a mediocre genetic test done – some measurements were taken and I had my eyes checked by an ophthalmologist for any telltale signs, but I didn’t meet enough of the criteria to be diagnosed with Marfan’s.
Life carried on as normal. I had gotten married, had my first son when I was 25, and just had my second son (with some high blood pressure complications) shortly before turning 27. A couple months later, I really started experiencing symptoms related to BAV – dizziness out of nowhere, unexplained sudden fatigue, and most likely the reason I had high blood pressure concerns during my delivery of my second son.
The lightbulb went off in my head and I could almost hear the words coming from that doctors mouth 8 years earlier. I immediately called up a cardiologist and explained my concerns, had a thorough visit with and EKG and followed up with an echocardiogram, only to confirm, again, that I had BAV, but now had a severe leak. This leak, otherwise known as aortic insufficiency, is a regurgitation of blood through my one-way aortic valve. The aortic valve is between the heart and the aorta, the main artery that supplies the rich, oxygenated blood to the rest of the body.
Now that I saw the results from the error of my ways, I chose to stay on top of my health. I first had calendared my biannual cardiologists’ checks, which would be an EKG and echocardiogram. The echo would measure my heart for any stress growth that could result from the insufficiency. I was put on a beta blocker and calcium channel blocker to help aid my heart in not feeling the pressure to pump so hard because of the regurgitation.
I trained for and ran my first half marathon. I would do 5k’s with ease. I loved being active and started participating in the American Heart Association’s Heart and Stroke Walk here in Boise. I also work for a large utility and they have always been so giving and supportive of the AHA and its mission to help Americans live longer and healthier lives. A little more on that in a few….
With my involvement in the AHA, I was able to attend the Go Red for Women Luncheon each year. The first year I attended, a female cardiologist spoke, and she just struck a chord with me. I had to meet her, and I felt like I had to switch to her being my cardiologist. So I did. She continued to monitor me for the next 6 years until an appointment in October of 2013 showed some great signs. I was 33 at the time. She said that my echocardiogram had showed no changes in my heart’s size, meaning no stress from the insufficiency, and that she felt comfortable for me to scale back visits to once a year. That was such encouraging news!
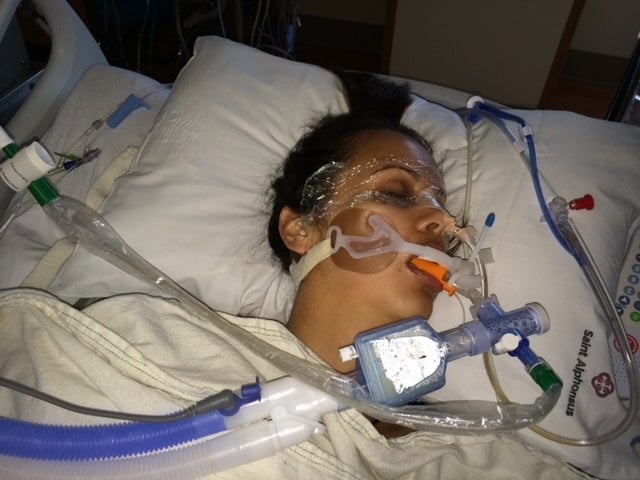
Just a few short months later in January of 2014, my family and I had a fun Saturday planned on the 11th. I had to work that morning for a few quick hours, then we were taking the boys up to the ski resort for ski lessons. My husband got up to go to the gym that morning, but because we had a busy morning planned, he opted to stay home. He went downstairs to start coffee and peruse the news online for a bit and came back up to bed. It was just before 6 AM. I was awake and he was asking me about my evening, as I had met up with some girlfriends the night before. I was reaching to grab my phone off the nightstand to show him pictures when my phone dropped to the ground. He asked if I was going to pick up my phone, when he heard a strange noise coming from me. He described it to be similar to someone choking. He jumped out of bed and flipped on the light to see me stiffened and in somewhat of a seizure-like display. He said my eyes were open and my pupils were fully dilated and I had absolutely no color to my face. He knew something was wrong with my heart. He grabbed his phone, called 911 and put it on speaker and checked for my pulse. Nothing. He started CPR.
I had gone into sudden cardiac arrest.
Table Of ContentsWhat is Sudden Cardiac Arrest?
Sudden cardiac arrest is the abrupt loss of heart function, breathing and consciousness. The condition usually results from a problem with your heart’s electrical system, which disrupts your heart’s pumping action and stops blood flow to your body.
Our boys were 8 & 6 at the time and our oldest had come into the room because he heard my husband yelling at me and the phone. He was scared and wasn’t sure what was going on. The 911 Operators (one was in training with the regular operator) conveyed the message to the fire department at the edge of our subdivision and they arrived about 5-6 minutes later. They weren’t relayed a sense of urgency, and my husband threw our bedroom window open and yelled at the first responders to hurry. Our oldest son had to run downstairs to open the door for the firefighters and hold our 90 lb lab from keeping them from coming in. Ada County Paramedics and Eagle Police followed behind them within a few minutes. The firefighters relieved my husband of the 6-7 minutes of CPR he had performed. They cut all my clothing off and proceeded to shock me with a defibrillator. I was found in V-fib, ventricular fibrillation, a fatal heart rhythm, that causes ventricles to ‘quiver’ and isn’t following the normal pumping rhythm, consequently causing blood to stop flowing through your body. The Eagle Police officers took both our boys into their room, closed the door, and talked with them to change the subject from that awful happenings in our room. My boys still remember talking to them about their ski clothes they had lined up, excited for their lessons that day.
I was shocked 4 times on my bedroom floor. My husband recounts asking the medic over me “what do you got? Anything?!” And the medic replying, “I’m sorry man, I don’t have anything.” Thankfully, that wasn’t the end. The supervisor was also on site, and reassurance was given that they were going to keep trying – so they put me on a gurney and put a LUCAS chest compression device on me. This lifesaving machine does chest compressions to the tune of 100 beats per minute all on its own. This allowed medics to maneuver my gurney down the twisty staircase, into the ambulance, and to the hospital, all without me missing any CPR during the transport.
I was taken to the local hospital in the town of Eagle where we live and was shocked 3 more times with a faint heartbeat returning. I was most likely injected with adrenaline, my husband remembers them giving me a shot of something when my pulse returned, but that was short lived as my heart stopped again. Then finally, the eighth shock was given, and my pulse returned and stayed. I was quickly transported to the main hospital in Boise, about 9 miles away. I was assessed by health care providers, given a full cath lab workup to see if I had blocked arteries (none), and then put into a medically induced cooling coma for two days. My body temperature was lowered to 88 degrees. The cooling helps to preserve any brain tissue that may have been damaged due to anoxia, or loss of oxygen, after my heart stopped pumping oxygen rich blood to my brain. I had also suffered a minor stroke. After the two days, I was reheated to the comfy 98 degrees we all know and before I was fully awake, an AICD – Automated Implantable Cardioverter Defibrillator – was installed in my chest above my heart with a lead in my heart. This would be my on-board back up, should my heart stop beating again.
The next minutes, hours, and days that followed were very difficult for my family members and friends. I was first told I may not have memory of basically anything – who my family was, why I was in the hospital, long term memory could’ve been affected, the doctors just couldn’t say where I’d be cognitively. My husband was told I could just be the shell of me but someone new inside. Just the most dismal information a spouse and sons could be told.
Miracles do happen though!
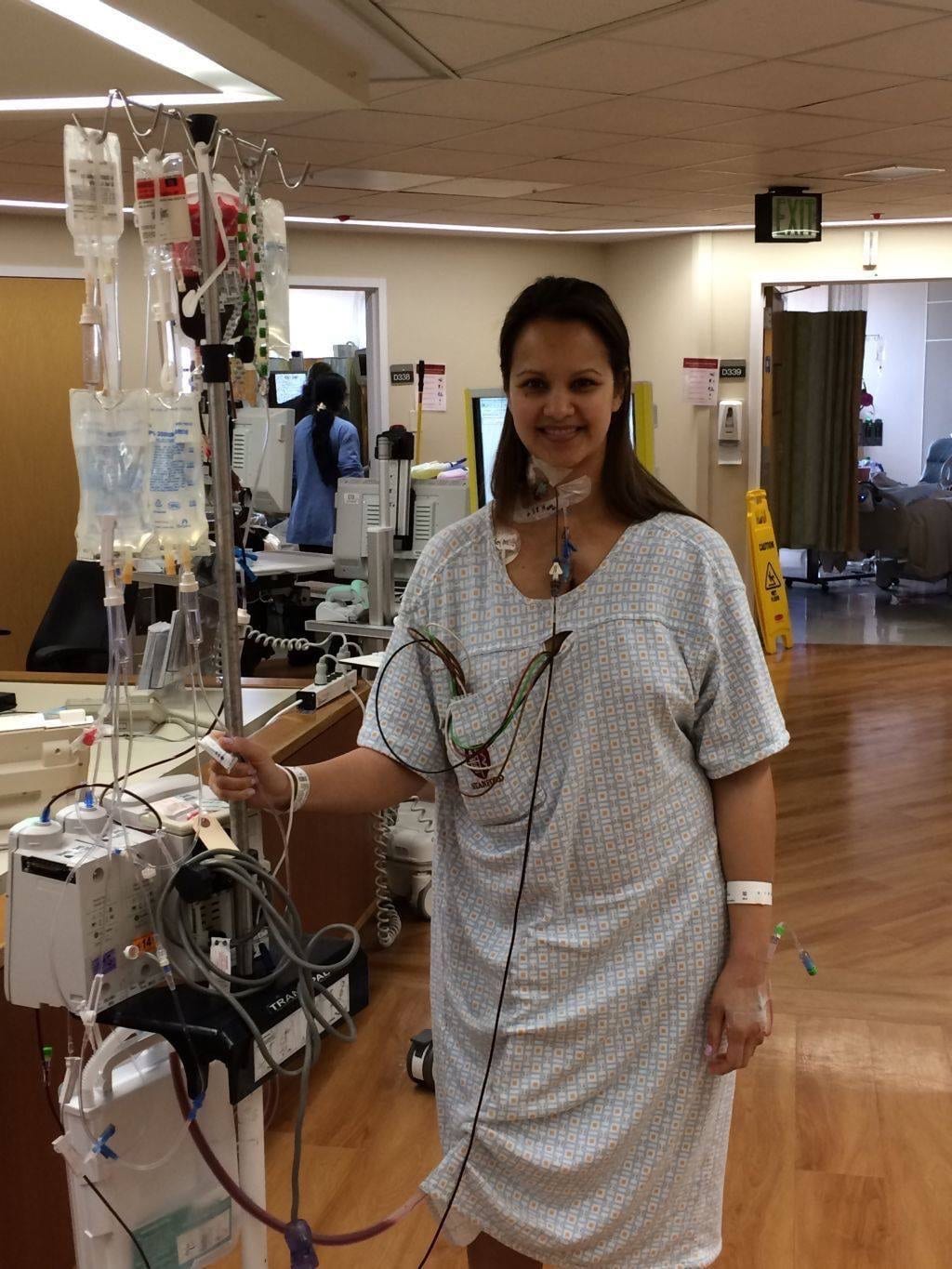
Sure, I got to be like Ten-Second-Tom in the movie 50 First Dates, one of my most favorite movies, by the way, for about a day. I improved each day. I was remembering family, remembering people who sent me cards, remembering long term memories and by the 6th day in the Cardiac Intensive Care Unit, I got to go home! I wasn’t out of the woods just yet.
What felt like the shortest seven weeks of my life, I went to Stanford University Hospital to have my aortic valve repaired. It experienced further damaged believed to have been due to the eight shocks. We met with my wonderful surgeon who was hopeful to do this surgery only done by a handful of doctors in the US at the time. My husband and I were at Stanford a few days before the surgery for pre-op tests and consultation with my surgeon, who discovered my valve was too far damaged for a repair and I would need a full replacement.
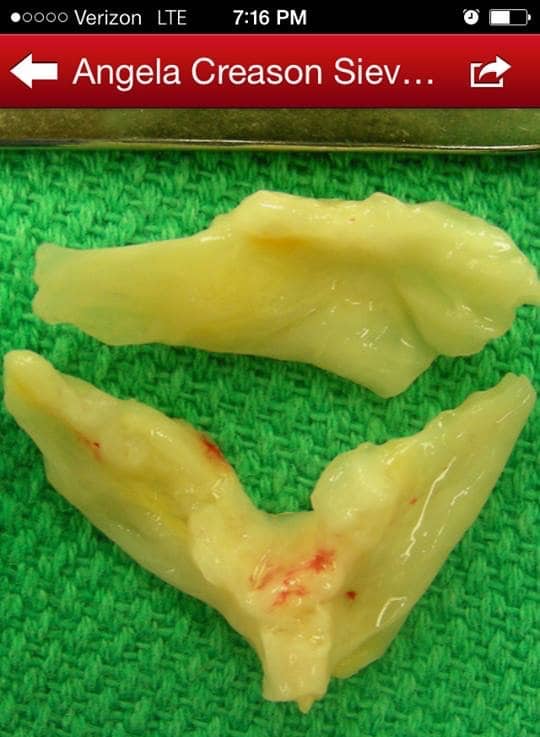
It was now the choice between a tissue valve from either cow or pig heart tissue, or a mechanical valve. A tissue valve meant no blood thinners, keeping the door open to having another child, not having to check INR – international normalized ratio – a number figured in a lab that measures the time it takes for your blood to clot, and needs to be checked regularly, anywhere from every week to every month, depending on the person. The con of the tissue valve, surgery to replace it again, approximately 10-15 years at the time of my surgery. The mechanical meant no further surgery, but checking my INR for the rest of my life because a clot that could form on the valve, could cause a stroke.
So open heart surgery was performed, taking about 6 and a half hours. My surgeon wanted me to have a smaller scar, so the team had to work harder in a smaller opening, adding some time to the surgery. I love and appreciate that they did that, but I would’ve proudly sported the full length scar.

I went home 5 days after surgery, but recovery was long and hard. It takes a while to get to using your arms again, and sneezing is NOT fun the first few weeks after. All OHS patients get a heart shaped pillow to use to squeeze when they get up from a seated position, so you don’t mistakenly use your arms to assist you, or when a sneeze makes its way to your nose, to help keep pressure on your chest at the incision site.
I returned to work just over 13 weeks after my sudden cardiac arrest and 6 weeks after my open-heart surgery. I followed up with more testing back at Stanford with a genetic panel to see if I had a genetic mutation that may have caused my cardiac arrest, but nothing was found. My cardiac arrest was an IVF, idiopathic ventricular fibrillation, meaning an underlying cause for my v-fib was never identified.
I started doing things because I felt lucky to be alive to even be doing them. Said yes to more random things I wouldn’t have normally done. I even ran, well, ran and walked, Robie Creek, the toughest half marathon in the northwest. I did it twice. The first time I did it in 3 hours 30 minutes. Nothing to brag about, but that uphill is brutal and I was worried my defibrillator might shock me! I talked with my electrophysiologist (heart rhythm doctor) and I was ok’d to run the flat and downhill, so I did Robie one more time to cut my time down significantly. I trained with some incredible friends that were so supportive and I ended up shaving off 30 mins off my first time!!
I became more involved with the American Heart Association and I stepped up to share my story countless times – I’ll tell it to anyone that’s interested. I was also the passion speaker for the Go Red for Women Luncheon the year after my cardiac arrest. I have volunteered for CPR day and to train CPR wherever a demonstration was needed. I worked with my employer to start using funds raised from our bake sales and silent auctions to purchase Automated External Defibrillator (AED) units for schools in our service territory. We have donated AED machines to rural schools where an AED portable device not only serves the school, but the community as well.
I’ve told everyone who asked how I was doing after my ‘heart attack’, the difference between a heart attack and a cardiac arrest. They are NOT the same, but one can lead to the other. I like to use the analogy of your heart being a house. You have plumbing and electrical in a house. A heart attack is when the plumbing has a problem (clogged/blocked coronary arteries). Cardiac arrest is where the heart’s electrical system has a problem (v-fib in my case). The biggest difference in these two events, is that a heart attack victim can be awake, talking, asking for help, etc. A sudden cardiac arrest victim instantly collapses with a loss of consciousness and is unresponsive. A heart attack victim can become unresponsive as well and some people can have a heart attack that leads to a cardiac arrest.
Knowing the difference between the symptoms of cardiac arrest and a heart attack can impact the victim – a sudden cardiac arrest victim needs immediate defibrillation and CPR, along with a call to 911. As in my case, my husband had to perform CPR on me. That’s just it.
Do you know CPR?
Are you prepared to help save the life of a loved one or friend, because that will most likely be the person that could need your help. Be ready. Learn CPR! Know where your closest AED is at school, sports venues, work, gym, grocery store. I make it a game whenever I’m in public places, to find the AED.
What is an AED?
An automated external defibrillator (AED) is a medical device designed to analyze the heart rhythm and deliver an electrical shock to victims of ventricular fibrillation to restore irregular heart rhythms to normal in the case of medical emergencies. Ventricular fibrillation is the uncoordinated heart rhythm most often responsible for sudden cardiac arrest.
Most of all, please be prepared. I was 33. Heart disease can strike anytime, and any age.

Thank you Angela, so much for sharing your story!
Support Angela in her support of AHA
If you are so moved, please feel free to support Angela as she continues to support the AHA to continue and increase heart health awareness and to encourage all to learn CPR. She will be participating in the 2022 Idaho Heart & Stroke Walk which takes place this coming weekend, Saturday, May 7, 2022.
I’ve already learned so much about about Sudden Cardiac Arrest through knowing Angela and I feel more aware of the warning signs and the importance of diagnosing heart problems early. I’ve also been surprised to learn that a heart condition is something that can affect young people – even young athletes – and while some people might be at higher risk due to a family history of cardiovascular disease, that is not always the case. The best way to prevent the risk of sudden cardiac arrest is to stay on top of your own health, get a regular physical exam, learn CPR and know the symptoms of SCA.
I encourage you to continue to educate yourself about the risk factors, symptoms of sudden cardiac arrest and even just an overall awareness of sudden cardiac arrest.
Have a plan in place should you ever need medical attention, and of course, making positive lifestyle changes can never hurt. Angela’s story has definitely inspired me to pay attention to my heart health!

Meet the author – Keri Lyn
The creative and frugal mind behind She Saved for over 12 years now, Keri Lyn shares her adventures in parenting along with her love for family travel, country living and brand marketing. A self-proclaimed “brand loyalist”, Keri Lyn is known for her strong and enthusiastic voice when it comes to the products and brands that she loves. She Saved has become a community for like-minded consumers who appreciate saving money, time and sanity by getting the best deals on quality products and experiences.